Ovarian Endometriomas vs Deep Infiltrating Endometriosis
Aug 1, 2017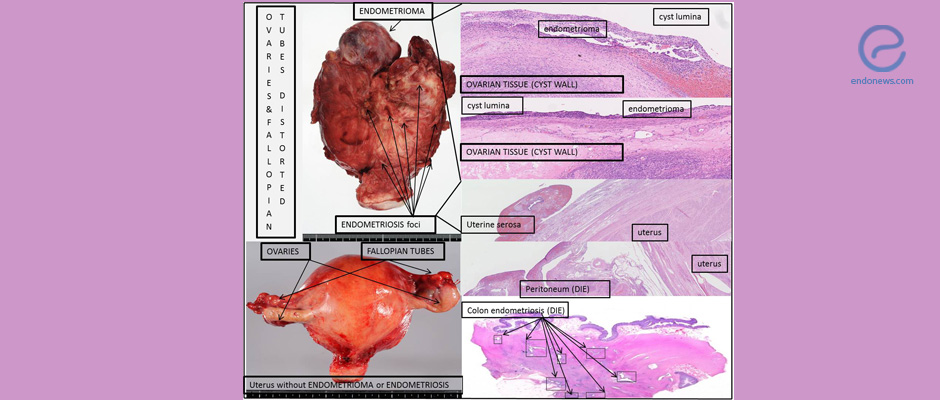
This study provided clues that may explain the pathogenesis of different endometriosis subtypes, deep infiltrating endometriosis, and ovarian endometriomas.
Key Points
Highlight:
- Ovarian endometriomas (OMA) and deep infiltrating endometriosis (DIE) appear different in histology. This study elucidates potential causes for their differences.
Importance:
- Lesion microenvironment differences between OMA and DIE may create their distinct histological features.
What's done here:
- Ectopic endometrial tissues collected from 25 women with OMA and 20 women with DIE. Control endometrial tissues obtained from 25 women without endometriosis.
- The expression of markers for epithelial–mesenchymal transition, fibroblast-to-myofibroblast transdifferentiation, smooth muscle metaplasia, fibrosis, vascularity, hormonal receptors, and epigenetic modifications proteins was evaluated using immunohistochemical analyses.
Data:
- Both lesions showed aberrant expression of proteins involved in fibrogenesis
- OMA and DIE showed different expression levels of hormone receptors.
- DIE lesions underwent more extensive:
- epithelial–mesenchymal transition,
- fibroblast-to-myofibroblast transdifferentiation, and
- smooth muscle metaplasia,
- higher fibrotic content and less vascularity compared to OMA.
- DIE showed significantly higher staining of markers suggesting progressive epigenetic changes.
Limitations:
- The difference between the OMA and DIE lesions within the same patients were not evaluated. This may be substantial as women with OMA and co-occurrence of DIE seem to have a more advanced condition.
Lay Summary
Ovarian endometrioma (OMA) and deep infiltrating endometriosis (DIE) have been described as two disease entities, although they are both characterized by endometrial tissue located outside the uterus. As OMA and DIE look different histologically, it is puzzling what cause their differences.
Importantly, among subtypes of endometriosis, OMA is most prevalently diagnosed, while DIE is thought to be less prevalent than OMA. Women with DIE, however, experienced more severe pain and challenging clinical management. Diagnosis for DIE includes endometriotic lesions infiltrating the peritoneum by greater than 5 mm.
This original research article by Liu et al. studied potential causes for the differences between OMA and DIE. Like all subtypes of endometriosis, these lesions undergo cyclic bleeding and repeated tissue injury and repair. The authors collected and compared ectopic endometrial tissue samples from 25 women with OMA, 20 women with DIE and control endometrial tissue from 25 women without endometriosis. These samples were studied using immunohistochemical analyses to evaluate the expression of a group of markers for epithelial–mesenchymal transition, fibroblast-to-myofibroblast transdifferentiation, smooth muscle metaplasia, fibrosis, vascularity, hormone receptors, and proteins involved in epigenetic modifications.
The data suggest that DIE lesions underwent more extensive epithelial–mesenchymal transition, fibroblast-to-myofibroblast transdifferentiation and smooth muscle metaplasia with significantly higher fibrotic content and less vascularity compared to OMA. These two subtypes of endometriosis also showed different expression levels of steroid hormone receptors: DIE showed reduced ER-β but increased PR-β levels than OMA. DIE samples had significantly higher staining of markers suggesting progressive epigenetic changes. Also, DIE lesions displayed less platelet aggregation but higher TGF-β1 staining. Collectively, these changes may determine the histology/morphologic differences between these two types of lesions, as well as their responsiveness to hormonal drugs.
Although more research is warranted to elucidate precisely how OMA and DIE develop, this study provided clues that may explain the pathogenesis of different endometriosis subtypes. Future work to evaluate the differences between the OMA and DIE within the same patients would be interesting, as OMA lesions with co-occurrence of DIE seems to have a more advanced condition.
In summary, this study showed similarities and differences between OMA and DIE lesions. The different histologic features of these lesions may be related to distinct lesion microenvironments. The study also suggested that progression of endometriosis may be linked to epigenetic changes.
Research Source: https://www.ncbi.nlm.nih.gov/pubmed/28718381
ovarian endometrioma deep infiltrating endometriosis DIE endometriosis subtypes

